Posts in Category: Uncategorized
honeysuckle flower – fever, sore throat
There is scientific evidence to back this up. For instance a 2018 systematic review of the biological properties of honeysuckle flower found that it has antibacterial, antiviral, anti-inflammatory, and anti-pyretic effects.(2) It was part of a combination of herbs given to “first-line medical staff” treating SARS in Beijing and none off these contracted SARS,(3) Further 23 Chinese Provinces have issued preventative programmes using herbal medicine against COVID-19, and a review of the history, research evidence, and current prevention programs concluded that people at high risk of contagion “would probably benefit from taking CHM formulae for prevention”.(3) In China these formulae are readily available in hospitals and pharmacies.
Yes. China once had to deal with epidemic diseases from the West.
Please note that under Australian Healthcare Advertising regulations, there is not enough high standard evidence to state that jin yin hua or Chinese Herbal Medicine in general effectively prevents infection by COVID-19, and no claim is made here that it does.
(1) Chen JK ‘How COVID-19 (2019-nCoV) is Currently Treated in China with TCM’
Retrieved 31/3/20 here:
(2) Yan-Ran Tang et al. Digital Chinese Medicine 1, 2, June 2018, 173-188. ‘Lonicerae Flos: A Review of Chemical Constituents and Biological Activities.’
Retrieved 31/3/2020 here:
(3) Lou et al. Chin J Integr Med 2020 Apr;26(4):243-250. ‘Can Chinese Medicine Be Used for Prevention of Corona Virus Disease 2019 (COVID-19)? A Review of Historical Classics, Research Evidence and Current Prevention Programs’
Retrieved 1/4/20 here:
R.I.C.E. for acute injuries and pain

Everyone knows to use R.I.C.E. for acute injuries, don’t they? I’m going to shake that up a bit.
I’ve posted that the guy who made up the R.I.C.E. acronym now agrees that ice does nothing to help injuries heal, and that others question whether compression or complete rest help either. So I couldn’t resist naming my liniment for acute injuries R.I.C.E. for Really Immediate Care Embrocation.
It is made from herbs that are traditionally used to relieve pain, and to reduce swelling and bruising. Notice that it doesn’t try to reduce inflammation, which is not a Chinese medicine thing, and which is now thought to be an important part of the healing process.
Use it immediately after an injury to muscles, tendons, joints, or bones, so long as there is no open wound in the area, and for the next three days or so or until the swelling subsides.
It’s packaged in small bottles as I hope you don’t need to use it often.
Women’s health & Chinese Medicine

How does Chinese Medicine look after women’s health?
For one, it has always recognised women’s difference, and that there needs to be specialised medicine for them. The earliest known medical texts discuss female anatomy and health, and many of the most important texts have chapters devoted to women’s health. As early as the 2nd century AD there were Chinese doctors who specialised in treating women, and today it is possible find doctors whose family have been doing so for as many as 37 generations. There are even acupuncture points that are used for complaints as specific as lower back pain during a period.
Conventional medicine is coming around to recognising the connection between mental and emotional states and health, but it’s fundamental to Eastern medicines. This is important for looking after everyone’s health, but maybe more so for women who are more likely to recognise and acknowledge their emotional state, than men who have been conditioned to ignore it. So women are often the ones who report an emotional factor to their doctor, and who used to run the risk of being labelled ‘neurotic’.
It’s notable that the Greek root of ‘hysteria’, is the word for uterus.
Chinese Medicine doctors don’t divorce emotional factors from their understanding of a person’s health, and even have a physiology of emotions that explains or predicts health problems. So regulating emotions is often part of treating an illness, and this can be important for women’s health, as they are often quite aware of how their emotions change in tune with their physiology. We have powerful but subtle tools to look after women’s health that we can use for the wide range of conditions that tend to be disregarded by conventional medicine, or treated with valium, the oral contraceptive pill, or surgery.
There’s a lot more we can do than suggest that a woman has a Bex, and a lie down.
A further strength of Chinese Medicine gynaecology is that it offers an understanding of a condition when there is no recognisable ‘organic’ pathology. This is what convention medicine looks for, either a recognisably diseased or damaged tissue, a microscopic pathogen, or a measurable imbalance in biomarkers. It then tends to treat gynaecological conditions with surgery, anti-biotics or anti-virals, or attempts to regulate hormone levels with the pill or an implant such as a Mirena.
Chinese medicine gynaecology offers solutions when there is no identifiable ‘organic’ disease. We use herbs and acupuncture to regulate periods that are too heavy or too light, debilitatingly painful, or are accompanied by back pain, headaches, or distressingly severe mood changes. We take particular care of women who have just had a child: we help them recover from the effort of growing a little human, help them with feeding, and give support during a time that does not always have the shiny happiness of the Insta feed.
There’s a bit more about Chinese Medicine gynaecology here by my mentor, Steven Clavey. He also shows some research covering its treatment of infertility, gynaecological pain, endometriosis, and menopausal symptoms.
The photo’s a bit naff. But apparently people like that sort of thing.
moxa punk bone broth

Who doesn’t know how to make bone broth these days? Or that hyperbolic claims of eternal youth aside it is awfully good for you. Despite there being as many bone broth recipes on the net as things you just wouldn’t believe so you must click now, I’m going to add my simple tips.
- Get a marrow bone or two. I prefer to use ones from organic certified cattle as I believe livestock tends to concentrate the bad shit that’s used to produce their feed, but this isn’t the place to start an argument about that. Use non-organic if you’re so inclined. Get the butcher to cut the bones into pieces so they’ll fit into your pot and so that the marrow can get out of them into the stock.
- Pre-heat an oven to 220 degrees C. Drizzle the bones with oil and season, then roast them for 10-15 minutes. This makes the stock a bit less ‘meaty’.
- Place the roasted bones and any pan liquids in enough cold water to cover them.
- Add an onion, a celery stalk and maybe a few leaves. Try not to get carried away with the vegetables. It’s bone broth. I used to add a carrot but found it caramelised so much over 24 hours that it turned the broth yellow and made it taste overwhelmingly of carrot.
- Bring to the boil.
- Once it starts simmering lower the heat. Skim off any floating scum, and do this again when it reforms.
- Simmer uncovered for as long as you can, 12 hours is a minimum, 24+ better. Covering tends to keep in the slightly whiffy aromas.
- Strain, cool, store, serve.
a miso soup recipe for bukowski
 Charles Bukowski was not a healthy living guy, but he made it to 72. He smoked, drank immoderately, didn’t pay much attention to what he ate, and despite his braggadocio about his boxing prowess and laboring ability, probably thought exercise dissipated the spirit. About the only healthy thing he did was avoid doctors after harrowing treatment for his acne.
Charles Bukowski was not a healthy living guy, but he made it to 72. He smoked, drank immoderately, didn’t pay much attention to what he ate, and despite his braggadocio about his boxing prowess and laboring ability, probably thought exercise dissipated the spirit. About the only healthy thing he did was avoid doctors after harrowing treatment for his acne.
Maybe someone of his robust stock would have got even older by following a bit of the standard advice for long, healthy life, or maybe without allowing himself to thrive spiritually he would have given up and withered away. The Moxa Punk’s approach could have helped him been a bit healthier physically, without robbing him of his spiritual vitality.
happy belly
 It seems to be common sense that our happiness affects our health, and consequently our digestion. And language has many examples of relating mental and emotional states with our alimentary tract. A shock can hit us in the guts, considered thinking is chewing things over or ruminating, we have gut feelings, and Australians say that things or people give them the shits. But while mainstream doctors may see this, conventional medicine’s empirical paradigm doesn’t allow the recognition of phemomena that it can’t measure, so there was often a tendency to label illnesses without clear somatic causes as neurotic. (1)
It seems to be common sense that our happiness affects our health, and consequently our digestion. And language has many examples of relating mental and emotional states with our alimentary tract. A shock can hit us in the guts, considered thinking is chewing things over or ruminating, we have gut feelings, and Australians say that things or people give them the shits. But while mainstream doctors may see this, conventional medicine’s empirical paradigm doesn’t allow the recognition of phemomena that it can’t measure, so there was often a tendency to label illnesses without clear somatic causes as neurotic. (1)
With new understanding of how gut flora can affect both our digestion and mood, and that conversely poor mental/emotional states such as depression can change the composition of our gut flora and impact our digestion (2), there is starting to be a way that conventional medicine can allow discussion of the link between how we feel and how well we digest things. There are even starting to be scientific papers with titles like ‘Gut Feelings’.
Chinese medicine has always been able to recognise this connection because its model is not entirely materialistic. Each physiological system is associated with an aspect of the psyche, and with an emotion that interferes with the proper functioning of that physiological system. So the system that transforms our food into nutrients is affected by worry, and the system that tries to stop us from getting uptight about life’s stresses gets stuffed up by anger and frustration. Just like the links between emotions and physiological function through gut flora, it works both ways, so poor digestion can bring more worry, and failure to relax can lead to more anger and frustration. To make things worse, these two physiological systems are linked, so weak digestion can make us less able to relax, and internalising stress too much, getting angry and frustrated, affects our digestion.

There are some traditional combinations of medicinals that illustrate how Chinese Medicine has always seen the link between our happiness and our digestion.
Tong x
Tong Xiie Yao Fang 痛瀉要方 (Important Formula for Painful Diarrhoea) was designed in 1481. It is designed to specifically address abdominal pain and rumbling with urgent diarrhoea that can relieve the pain. This is a manifestation of weak digestion that has been disrupted by pent-up emotions. Not surprisingly it is the basis of many prescriptions for IBS with pre-dominant diarrhoea and it has been found that it could be superior to routine pharmacological treatment for this condition.(3)
 Conversely, anger, resentment, frustration, pent-up emotions, and not letting things go may manifest physically as impeded elimination. Liu Mo Yin 六磨湯 is a combination of medicinals that addresses constipation that results from us letting our emotions block us up quite literally. It uses herbs that gently move things through the digestive tract, but which also assist flow generally, in the sense that they relieve the general mental and physiological stagnation that is both the result of us not properly dealing with stress, and a contributing factor to our inability to do so.
Conversely, anger, resentment, frustration, pent-up emotions, and not letting things go may manifest physically as impeded elimination. Liu Mo Yin 六磨湯 is a combination of medicinals that addresses constipation that results from us letting our emotions block us up quite literally. It uses herbs that gently move things through the digestive tract, but which also assist flow generally, in the sense that they relieve the general mental and physiological stagnation that is both the result of us not properly dealing with stress, and a contributing factor to our inability to do so.
More immediately the way we eat can help us digest better. We should be happy and relaxed, ideally with good company, and the Chinese even think it best to talk about how delicious the food is. Save the horror movies, the news and current affairs, political discussion and family arguments for after dinner.
-
Though for some years a link was made between personality type and cardiovascular disease, without there being a convincing explanation of how they could be linked. Of course this link was disputed by many.
- JA Bravo, M Julio-Pieper, P Forsythe, W Kunze, TG Dinan, J Bienenstock, JF Cryan. “Communication between gastrointestinal bacteria and the nervous system” Current Opinion in Pharmacology Volume 12, Issue 6, December 2012, Pages 667-672
- Yun-kai Dai, Dan-yan Li, Yun-zhan Zhang, Meng-xin Huang, Yi-le Zhou, Jin-tong Ye, Qi Wang, Ling Hu. ‘Efficacy and safety of Modified Tongxie Yaofang in diarrhea-predominant irritable bowel syndrome management: A meta-analysis of randomized, positive medicine-controlled trials.’ PLOS Published: February 6, 2018 https://doi.org/10.1371/journal.pone.0192319
plantar fasciitis
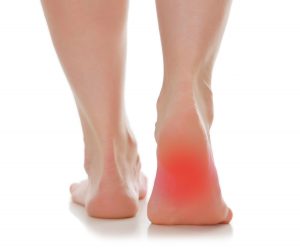
Heel pain is often from plantar fasciitis, a reactive condition of the tendons in the sole of the foot. This is characteristically most painful with the first few steps after getting out of bed, or after prolonged rest, and the pain reduces after walking around a bit. Pulling the toes up towards the top side of the foot and the shin, or pressing around the heel pad of the sole close to the back of the foot (over the bone known as the calcaneus) may reproduce the pain.
Acupuncture is a good treatment option for plantar fasciitis, and the treatment is helped by the use of herbal foot soaks and physical therapy.
dry-needling
What’s the difference between dry-needling and acupuncture? It depends who you ask. Someone who thinks they are different may say that acupuncture is part of the Chinese Medicine paradigm of diagnosis and treatment, and involves putting needles into traditional point locations arranged as channels; wheras dry-needling is part of a western paradigm of treating muscles and tendons. But it’s not that simple, and a closer look shows that what some people call dry-needling is really acupuncture.
magnolia buds
 Magnolia buds are out in Melbourne. We use them for the nasal congestion of colds,sinusitis, and hayfever. The hairs can be a little irritating though so the buds are put in cloth bags when we brew tea from them.
Magnolia buds are out in Melbourne. We use them for the nasal congestion of colds,sinusitis, and hayfever. The hairs can be a little irritating though so the buds are put in cloth bags when we brew tea from them.
The drawing is from “Famous Flowers of China”
in complete diets foods complement each other – here’s a dashi recipe
Go for complete diets not cherry picked ‘superfoods’, and whole foods rather than supplements.
As I mentioned before, when I used to ask the redoubtable Phillip Chu about various supplements he would reply, ‘Why? Trust your food!”
Chinese medicine prefers balanced diets with a range of healthy foods to over-emphasis on ‘superfoods’ and obsessive consumption of them, and it’s not particularly fond of extracted supplements.
But what about all those ginseng, royal jelly, and reishi mushroom pills in the Chinese pharmacy?’ you ask. While, just because someone wants to sell it to you doesn’t mean taking it is a good idea. The confusing and complicated story of soy and konbu supplements could be illuminating here.
You could write scientific papers about this but let’s try to keep it simple.
People noticed that the Japanese tend to be healthier than a lot of Westerners, and had a lower incidence of certain cancers such as breast cancer, but that the incidences of these in Japanese living in the West were higher. This made people think that diet could be a factor, and the higher consumption of soy products by Japanese was obvious. This led to recognition that soy products contain compounds called phytoestrogens that bind to cells in the same way that oestrogen does.The next thing you know there are pills and supplements containing these phytoestrogens with a number of claimed health benefits.
This is where it gets complicated: it is not clear whether the pytoestrogens stimulate the same responses as oestrogen does, or whether they reduce or regulate the effects of oestrogen in the body; and that this differs in various parts of the body, in people of different ages, and even between people with different lifelong or even intergenerational consumption of soy products.This is important because some cancers are affected by oestrogen, so would be encouraged if phytoestrogens acted like oestrogen, but weakened or prevented if they blocked the action of oestrogen.It is also possible that because they act like a hormone, but but are different from oestrogen, phytoestrogens could change the behaviour of cells in the body in unknown ways that oestrogen doesn’t. A further possible complication is that while soy products contain a number of phytoestrogens that could have slightly different actions and moderate or regulate the effects of each individual phytoestrogen, supplements generally contain one or two.
Even though Japanese women are less likely to get breast cancer than Westerners, it is was discovered that Western women who took soy supplements had increased levels of a hormone, IGF-1, that is associated with an increased risk of breast cancer. It turns out that consuming seaweed, as Japanese people also do, moderates the effect of soy on IGF-1 levels. [2]
Others have suggested that consuming soy may affect thyroid function, but this is unlikely if the dietary intake of iodine is sufficient, and seaweed which is an excellent source of iodine is recommended for those who consume soy products. [3]
It’s a mutually balancing relationship. Which is fortunate because konbu supplements with a range of claimed health benefits are popular – konbu is the Japanese word for kelp, a seaweed. Consuming too much seaweed can increase iodine levels so much that the thyroid becomes overactive and affects health. That this can happen has even been covered by the media. But in Japan where people consume a lot of seaweed, they do not tend to have excessive iodine levels, and it’s because of the soy consumption. It seems that consuming soy can moderate the uptake of iodine from seaweed.[4] Just as some possible adverse effects of eating too much soy are balanced by seaweed, the effects of eating to much seaweed are balanced by soy.
The Japanese have a variety of ways of using seaweed. Dried flakes of seaweed are sprinkled on rice, or made into a seasoning mix with sesame seed, dried tuna flakes, and salt as in furikake, or chopped and dressed as a seaweed salad. Sushi is wrapped in sheets of dried seaweed called nori, and this can also be shredded and added to rice. Then there’s the seaweed stock usually made from konbu, dashi, which is the base of miso soup and can be used to add savoury yumminess or umami to just about anything.
Some people prefer to use Japanese grown seaweeds as they think Chinese seaweeds are grown in more polluted waters.
Dashi is usually made with bonito flakes or katsuobushi, and these add a wonderful smokiness to the stock, but headless dried anchovies that are available from Chinese grocers are an easy and cheap alternative. I once made a dashi using the anchovies in oil that were in the fridge.
750ml room temperature water
15g konbu – about 12cm square
2 dried shitake mushrooms, soaked for 10 minutes
9g katsuobushi – a handful or so
Wipe the konbu with a damp cloth. Put it and the shitake mushrooms in water and heat until it is just starting to steam. Take it off the heat and rest for 1 hour, then take out the konbu. Heat again until it just starts bubbling, turn off the heat and drop the katsuobushi in and steep it for 5 minutes. Strain off the stock.
This can be make without the rest but the umami flavour will not be as developed. If using headless anchovies use a big handful and they can be simmered for a few minutes after the konbu is taken out.
You can off course, make miso soup from your dashi stock, and put some tofu in it.
- Rietjens I, Louisse J, and Beekmann K. The potential health effects of dietary phytoestrogens British Journal of Pharmacology 2017;174 1263-1280.
- Teas J, Irhimeh MR, Druker S, Hurley TG, Hébert JR, Savarese TM, Kurzer MS. Serum IGF-1 concentrations change with soy and seaweed supplements in healthy postmenopausal American women. Nutr Cancer. 2011;63(5):743-8.
- Messina M, Redmond G. Effects of soy protein and soybean isoflavones on thyroid function in healthy adults and hypothyroid patients: a review of the relevant literature.Thyroid. 2006 Mar;16(3):249-58.
- Munehiro Yoshida, Ayumi Mukama, Ryota Hosomi, Kenji Fukunaga. Soybean Meal Reduces Tissue Iodine Concentration in Rats Administered Kombu Biomedical Research on Trace Elements 2017;28(1) 28-34





